MEDICAL DEVICE INSPECTION SOLUTIONS
You’ve invested time, money and energy into quality assurance while doing your best to keep costs low and productivity high. But is your quality system doing its best for you?
Manual packaging and handling procedures, outdated data-management systems and the constant risk of human error can too easily compromise the quality and integrity of medical devices, putting patient health and safety at risk.
As the industry moves toward more stringently controlled, connected medical devices, OPTEL’s innovative, turnkey vision system and digital traceability solutions can help you optimize safety and security with minimal disruption to precious productivity time.
OPTEL’S MEDICAL DEVICE SOLUTIONS INCLUDE:
Quality Assurance and False Rejects
On average, one company per year sees a 10-percent drop in share price after a single, major quality event, and the risk of long-term reputational damage is real.
Recall Reduction and Management
Non-routine quality events such as recalls cost the industry an average of up to $5 billion per year, yet many manufacturers still rely on monolithic systems that actually slow their ability to track and manage recalls.
Tracking Devices Up to the Patient
In the event of a recall, tracking medical devices up to the patient is critical, yet some manufacturers don’t even have a warehouse management system (WMS) in place to tell them where their product is in the supply chain.
Complying with UDI Regulations
Develop a future-proof UDI strategy and be prepared to adapt to evolving requirements across countries and regions worldwide.
In the wake of media reports about medical device recalls, defects and government oversight, many regulatory bodies are now drafting or enacting tougher controls over medical devices. Failure to comply is not an option.
MORE THAN 30 YEARS OF EXPERTISE
MARKET-LEADING TECHNOLOGY BASED ON INNOVATION, PERFORMANCE, INTEROPERABILITY AND RELIABILITY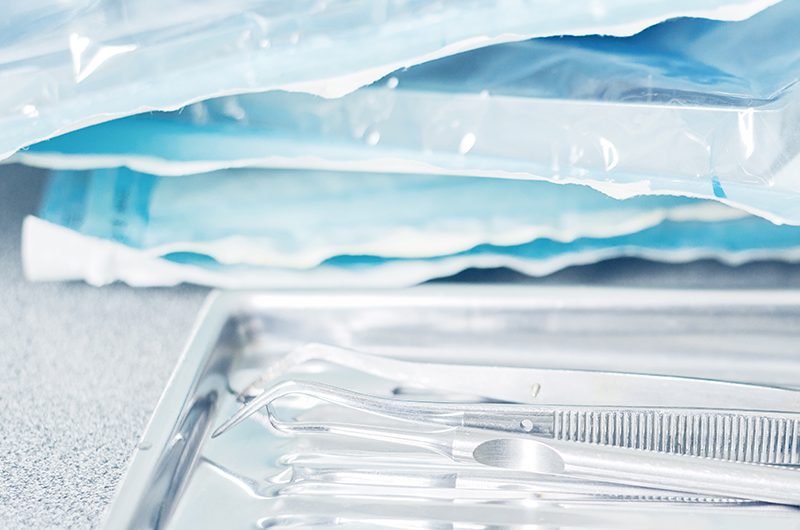
KIT AND TRAY INSPECTION
In addition to detecting component presence, our systems use metrology to detect millimetric differences in the general attributes of the items contained in kits and trays.
Contact Us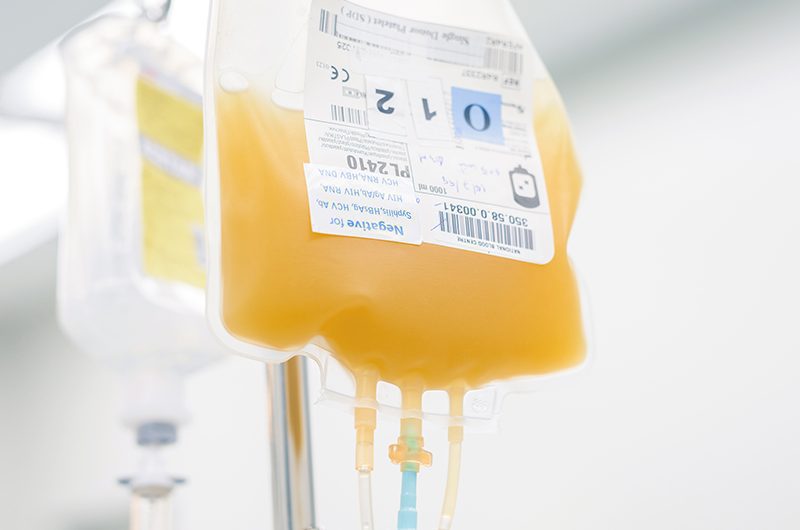
LABELING AND PRINTING INSPECTION
Inspect printing on packaging materials, including flexible web, Tyvek, paper, foil, pouches and more. Detect label presence and characteristics, artwork and variable data, barcodes and grading to comply with.
Learn more
Medical Device Counterfeiting
Case StudyDISCOVER THE RIGHT TRACEABILITY SOLUTION FOR YOUR INDUSTRY

Pharmaceutical
Track-and-trace systems for the pharmaceutical industry
Wholesalers and Distributors
Serialisation solutions for EU FMD compliance
Manufacturers
Track-and-trace solutions to help comply with all upcoming regulations
CMOs and CPOs
Serialization solutions to help achieve compliance
3PLs and Repackagers
Achieving compliance without disrupting the supply chain
Hospitals and Pharmacies
Solutions for healthcare providers and pharmacies